
ALLY’s powerful imaging technology maps the eye with unsurpassed detail. Robotic image analysis, based on learnings from thousands of cases and fueled by a built-in NVIDIA GPU, increases the accuracy of anatomical surface detection for precise treatment planning.

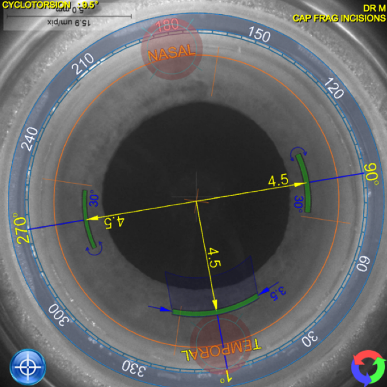
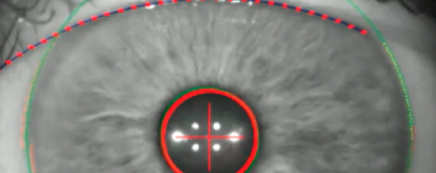
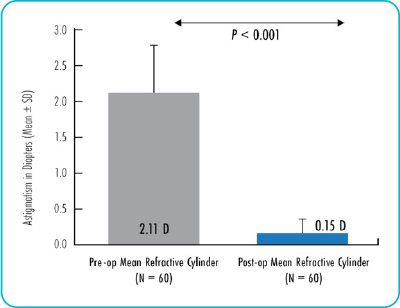
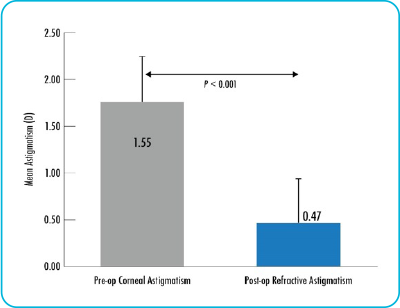
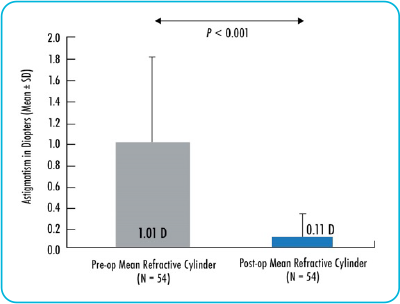
ALLY’s proprietary technology delivers a new level of precision and accuracy to improve astigmatic management.
99% of patients experienced cyclorotation and subsequent adjustment in at least 1 eye (n=354 eyes)6
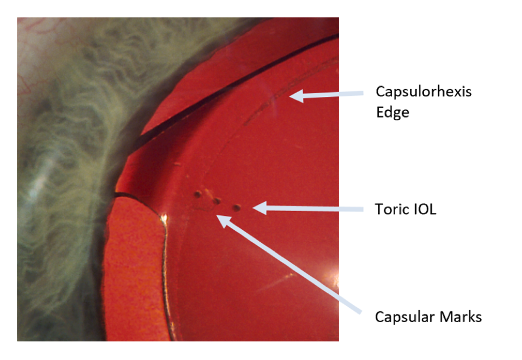
Guided by ALLY’s powerful robotic imaging technology and iris registration, IntelliAxis Refractive Capsulorhexis® incorporates small tabs on the capsular rim to clearly identify the intended axis both intra- and postoperatively.
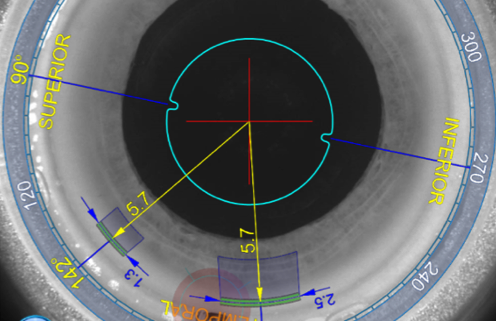
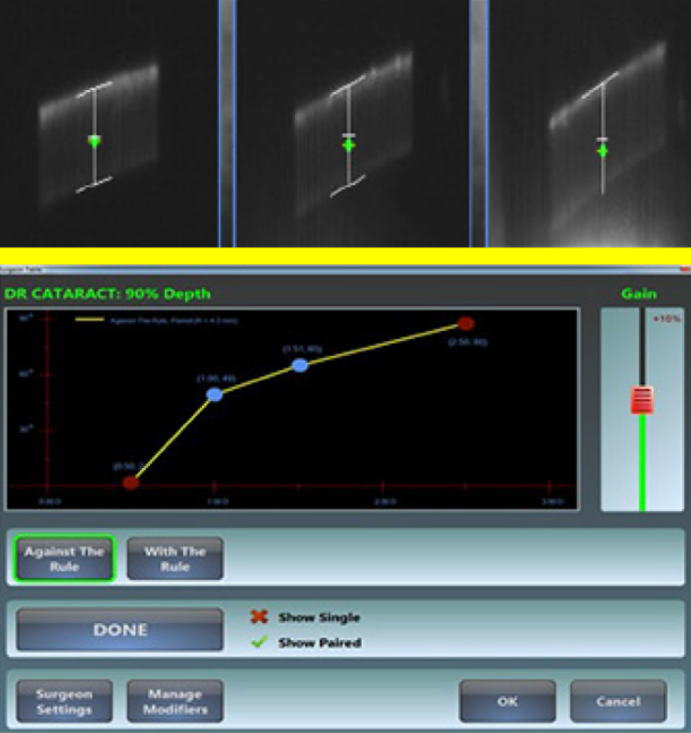
Optimized arcuate incision planning
ALLY offers convenient, one-touch arcuate incision planning based on the surgeon's most current pre-programmed nomogram data.
Smart corneal incisions
To further precision, ALLY monitors the position of the cornea before each cut to ensure the precise location and depth of every incision (paracentesis, entrance, and arcuate).
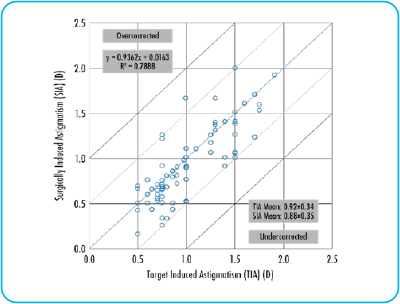
Surgically induced astigmatism (SIA)
The ALLY System automatically modifies incision parameters to account for SIA and residual astigmatism entries.
Customizable capsulorhexis
improves ELP
For better effective lens positioning (ELP), which is critical for premium IOL outcomes, ALLY allows surgeons to customize the size, shape, and position of the capsulorhexis to optimize for the IOL being used.
100% round, free-floating capsulotomies7,8
Further, ALLY's robotic laser precision significantly improves the accuracy and repeatability of capsulotomy construction and the predictability and stability of postoperative refraction.
LENSAR’s laser systems provide optimization of laser fragmentation patterns reduces both endothelial cell loss and inflammation, enhancing rapid visual recovery.9

*Based on surgeon preference
References
